Ticks and Tick-Borne Diseases
APPOINTMENTThe Scoop on Ticks and Tick-Borne Diseases
Who should worry about ticks?
The short answer? Everyone.
The prevalence of ticks and tick-borne diseases are rapidly increasing in New York. In Chemung County, 1 in 8 dogs is diagnosed with Lyme disease. Any pet who has access to the outdoors may be exposed to ticks. People can also bring ticks inside on their clothes, and outdoor dogs may bring ticks and other parasites back into the house where indoor-only pets (like cats) may be affected.
One of the most common consequences of a tick bite is Lyme disease, although ticks transmit many different diseases, including anaplasmosis and ehrlichiosis, which affect the blood cells.
Interested in regularly updated statistics? Visit www.capcvet.org to explore the parasite prevalence maps by state and by county.

How can I prevent Lyme Disease and other tick-borne diseases in my pets?
- Year-round use of tick prevention (see below for our recommendations)
- Lyme vaccine for dogs
- Check yourself and your pets daily for ticks and remove them as soon as possible. It takes between 24 to 48 hours for a tick to transmit Lyme disease, but other diseases may be transmitted in as little as 3 hours. A flea comb can be helpful in finding ticks.
I found a tick on my pet! What do I do now?
- Remove any ticks with a Tick Twister or tweezers. Learn how to use a Tick Twister here: https://www.youtube.com/watch?v=9N_GmW0G3IE. Stop by our office to pick up a set of Tick Twisters today!
- Do NOT use soap, alcohol, or oil on the area or try to burn the tick off. Do not squeeze the body of the tick. This will only lead to an increased risk in transmission of diseases. If you have trouble removing a tick from your pet, please call your veterinarian. We would be more than happy to have one of our veterinary nurses help you remove any ticks.
- If the body of the tick has already been removed and the mouthparts remain in your pet, don’t panic! The embedded mouthparts are unlikely to be removed if the rest of the tick is gone. They do not cause additional harm and will work their way out on their own.
- A tick bite may cause a mild reaction or bump at the site of attachment. This may persist for several weeks and will typically resolve on its own. If the area appears to be infected or your pet is itching at it, please contact your veterinarian.

When should we test for tick-borne diseases?
Once the tick has been removed, we recommend using a good tick preventative and having blood testing performed about one month after tick exposure. Most tick-borne illnesses (like Lyme disease) produce antibodies that will be picked up on a blood test 4 weeks after exposure to the tick. If your pet starts to show clinical signs of Lyme disease (as noted below), please call your veterinarian so testing and treatment can be performed sooner.
What are the signs of Lyme disease?
- Shifting lameness (lameness that switches from one leg to another)
- Fever
- Lack of appetite
- Lethargy
- Arthritis
- Reluctance to rise
- If left untreated, Lyme can cause life-threatening kidney failure and very serious joint disease
- Since some pets may be infected with a tick-borne disease but never show clinical signs, testing is always recommended one month after tick exposure.
Lyme vaccine for dogs
At Lake Road Animal Hospital, we strongly recommend the Lyme vaccination as part of your dog’s core vaccines and preventative care. This vaccine is a series of two immunizations 3 to 4 weeks apart, then is boosted yearly.
Tick prevention
There are so many flea and tick products available – and they are not all created equal. We understand that choosing the best preventative can be an overwhelming task, so let us help you when making this important decision! Using a veterinary approved product from your veterinary office or our home delivery pharmacy ensures that your pet is receiving the best quality care and a product suitable for his or her medical history and lifestyle.
Which tick preventatives are best?
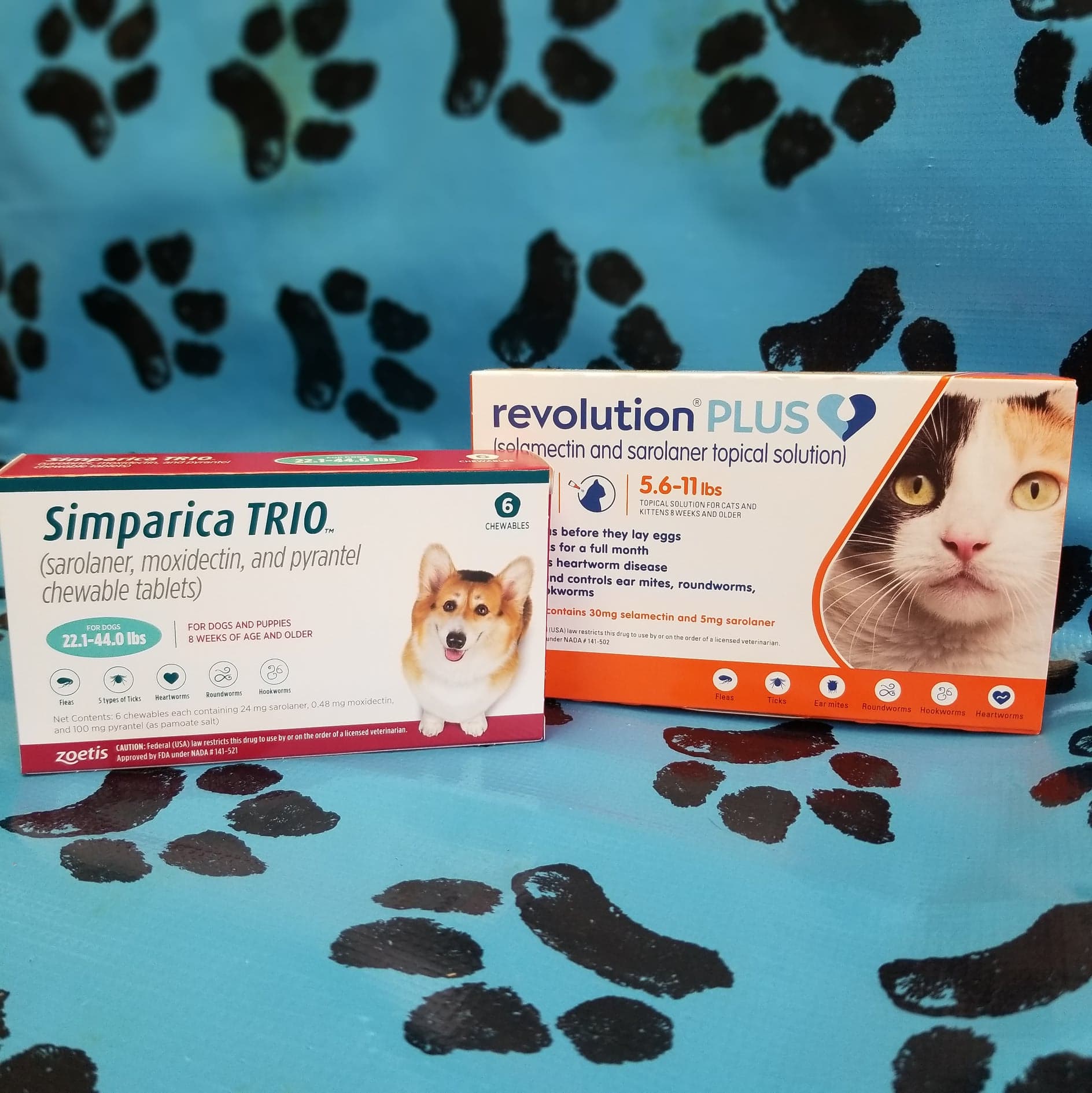
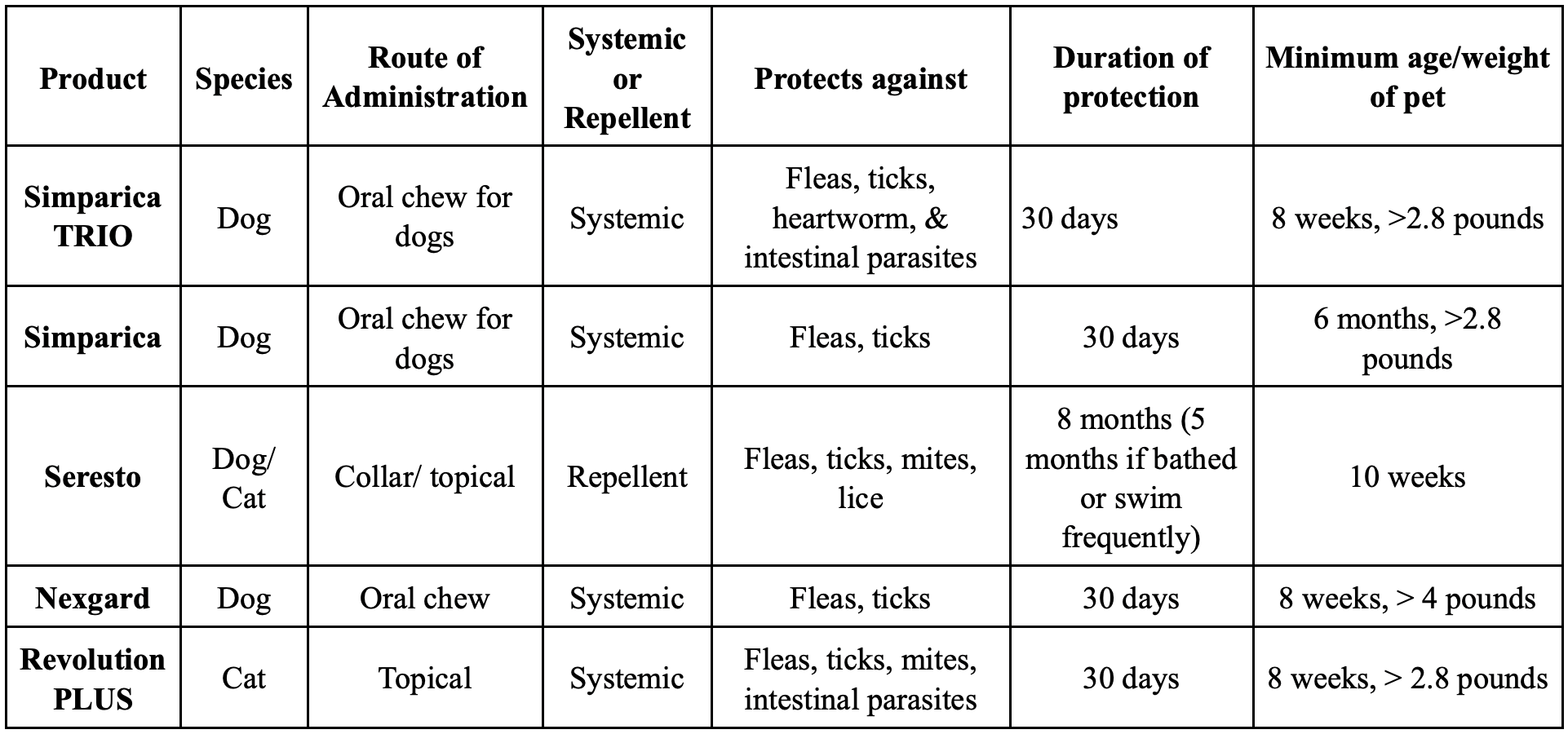
Oral and some topical preventatives are distributed throughout your pet’s body to give systemic protection. Systemic products are waterproof, safe for your dog or cat, and kill ticks soon after they bite your pet.
Products with repellency (like the Seresto Collar) are best when used in addition to a systemic preventative. This dual protection is best when your pet has a higher chance of encountering ticks (such as camping, hiking, or running through the woods).
The Seresto collar distributes the product to your pet’s skin and fur, but each time your pet swims or is bathed, the product is washed off, and the collar must release more of the active ingredient, depleting the collar sooner than the labeled 8 months. Pets who are bathed or swim more than once per month only receive 5 months of protection from fleas and ticks with the Seresto collar.
WARNING – Topical tick products for dogs and many over the counter products are TOXIC to cats and can be fatal. Always check with your veterinarian and read your product label before giving or applying preventative products to your pets.
When should my pet be on a flea, tick, and heartworm preventative regimen?
Ticks can become active when it is as cold as 36 degrees. Cold winters cause ticks to become dormant, but at first sign of a mild thaw, they can become active and attach to you or your pets. At Lake Road Animal Hospital, we have removed ticks from patients in January! Year-round protection is crucial, although spring and fall are the most heavily populated tick seasons. Spring brings the nymph ticks – no larger than a poppy seed – while the adults tend to be more active in the fall.
But I’ve never seen a tick on my pet!
Many pet owners are baffled if their pet tests positive for Lyme disease or other tick-borne disease because they have never seen a tick on their dog or cat. It is very easy to miss seeing a tick that is the size of a pinhead, especially when our pets have such thick fur coats. This is why tick preventatives are so important. We often can not see the ticks to take them off our pets before they transmit disease!
Free Tick Testing
If you find a tick on your pet, you could have the tick tested for free and help with research at the same time! After submitting a tick, you will receive an email with the type of tick submitted and the pathogens it could transmit. This data is collected to investigate the types of ticks in different geographic areas and to categorize the diseases that could be transmitted by the ticks. Click the link below to find the submission form and mailing address to Oklahoma State University’s research center.
Website: www.showusyourticks.org
Email ticksonpets@okstate.edu with any general inquiries or questions
Lyme Disease in Dogs
Diagnosis of Lyme Disease
- Blood testing (4dx) in clinic is recommended annually and 4-6 weeks after tick exposure to screen for Lyme disease, anaplasma, and ehrlichia.
- If your pet tests positive on the 4dx, this indicates that antibodies are present, but it does not specify the degree of infection. A confirmation blood test (C6) is sent out to our lab to check the antibody level. This value helps our veterinary team to determine a treatment plan for your pet.
- If your pet’s antibody level (the C6 test) is low and does not indicate that treatment is recommended, it is best to vaccinate your dog for Lyme disease immediately.
- Since Lyme disease can affect the kidneys, urine testing is performed in clinic. This testing helps to indicate the health of the kidneys.
Treatment
- Doxycycline is the most common antibiotic used to treat Lyme. This antibiotic is given for at least one month and is best given after a full meal since it can cause stomach upset. Avoid dairy products when giving this medication, as dairy interferes with its effectiveness.
- Medical therapy to treat pain, kidney disease, lameness, and lack of appetite as needed
- Kidney disease requires more extensive long-term treatment with antibiotics, fluids, and kidney protective measures
Follow up care
- Pets who have been infected with Lyme disease do not obtain immunity from future infections, so vaccinating for Lyme disease and keeping your pet on an excellent tick prevention regimen is essential for keeping them healthy. We strongly recommend vaccinating for Lyme disease as soon as the antibiotic therapy is finished.
- A C6 titer is tested 6 months after treatment to monitor response to antibiotics.
- Monitor at home for lameness, lethargy, excessive urination or drinking, or inappetence, which can occur if another tick reinfects your pet or the old infection was not resolved.
Lifetime expectations for your pet
- Some pets, after recovering from the infection, will show a positive result on the in-house 4dx test for months, years, or even the rest of their lives.
- Yearly monitoring of the C6 titer will help us to determine if a positive 4dx result is from antibodies from the previous infection or from a new infection. If the antibody level is low, then we continue preventative measures and simply monitor for signs of illness.
- In humans, there are many long-term effects of Lyme disease. However, in most dogs, Lyme disease presents as an acute infection and rarely becomes a chronic condition if treated in a timely manner.
Can Lyme disease be passed between pets or to people?
Lyme disease is only transmitted from ticks, and not from one dog to another or to a human from a pet. Although you cannot get Lyme disease from your pet, since you and your pet live and walk in the same areas, it is possible that you could also have been exposed to ticks carrying diseases as well. If you have any concerns about your health or wish to be tested for tick-borne diseases, please contact your physician.

Address

Hours
Mon: 8:00 am – 6:00 pm
Tue: 8:00 am – 6:00 pm
Wed: 8:00 am – 6:00 pm
Thur: 8:00 am – 6:00 pm
Fri: 8:00 am – 5:00 pm
Sat & Sun: Closed

Contact & Connect
Phone (call or text): 607-733-6503
Fax: 607-733-3656
Email: lakeroadradiography@gmail.com
Facebook
Instagram
Directions from Corning:
- Take 17/86 east towards Binghamton
- Take Exit 53 (Horseheads) exit and stay to the right
- Go through two lights, and at the third light take a right onto South Main, this turns in to Lake Road
- The hospital is ~1.5 mile on the right
Directions from Elmira – local roads:
- Take Church St. or Water St.to the Madison Ave Bridge
- Take a left on to Madison Ave, this turns in to Lake St, and then to Lake Rd.
- Follow Lake St. to Lake Rd. past Curly’s Chicken, the hospital is ~1/2 mile on the left
Directions from Elmira – highway:
- Take 17/86 West towards Horseheads/Corning
- Take Exit 54 towards Horseheads/Rt 13
- Stay to the left to exit towards Horseheads
- At the light, take a left on to South Main which turns in to Lake Road
- The hospital is ~1.5 mile on the right